Key Takeaways
- Endoscopy is a vital diagnostic and preventive procedure used to evaluate the digestive tract, detect abnormalities, and guide treatment.
- Sedation can improve patient comfort, reduce anxiety, and facilitate procedure completion, but carries some risks.
- Unsedated endoscopy avoids sedation-related complications and allows faster recovery but may increase discomfort and procedural stress.
- Understanding the benefits, risks, and preparation requirements of each approach helps patients make informed decisions in consultation with their healthcare provider.
Endoscopy is a common medical procedure used to examine the gastrointestinal tract, identify abnormalities such as inflammation, ulcers, or tumors, and guide therapeutic interventions [1]. Patients often face the choice of undergoing endoscopy with sedation or without.
Endoscopy with sedation is generally safe for most patients and improves comfort and procedural success, while unsedated endoscopy avoids medication-related risks but may involve more discomfort and anxiety.
Making the appropriate choice depends on the patient’s medical history, tolerance for discomfort, anxiety levels, and the complexity of the procedure.
What Is Endoscopy?
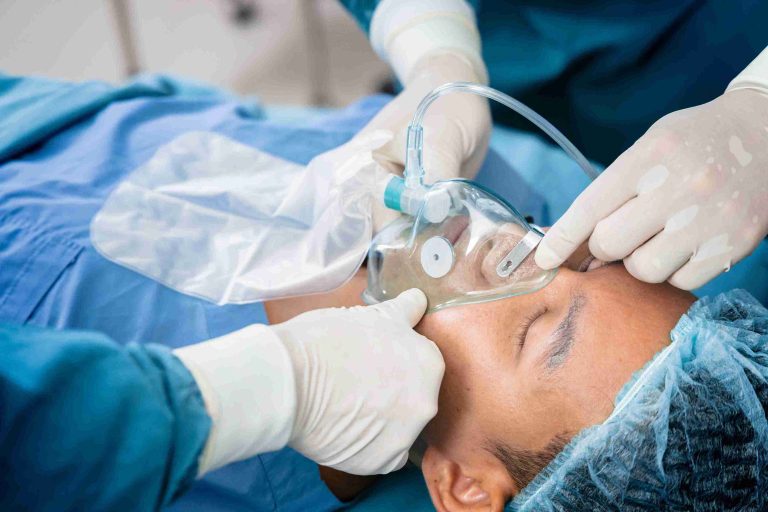
Endoscopy involves inserting a flexible tube equipped with a camera and light into the gastrointestinal tract, typically through the mouth (upper endoscopy) or rectum (colonoscopy or sigmoidoscopy), allowing physicians to directly visualize and assess the digestive tract.
Endoscopy can be diagnostic—used to detect abnormalities—or therapeutic, such as removing polyps, taking biopsies, or treating bleeding lesions. Patients may undergo the procedure with sedation, where medications induce relaxation or sleep, or without sedation, where the patient remains awake and alert.
Benefits of Sedated Endoscopy
Sedation improves patient comfort and cooperation during endoscopy [2]. The most commonly used forms of sedation include:
- Conscious sedation: Patients remain responsive but relaxed.
- Deep sedation / general anesthesia: Patients are fully unconscious and unresponsive.
Advantages of Sedation
- Reduced Discomfort: Sedation minimizes pain and gagging sensations, making the procedure more tolerable.
- Lower Anxiety: Patients with procedural anxiety benefit from sedation, reducing stress and improving overall experience.
- Improved Procedural Success: Relaxed muscles facilitate easier navigation and more complete visualization of the gastrointestinal tract.
- Safer for Complex Procedures: Sedation is recommended for longer or technically difficult endoscopies, such as therapeutic interventions.
While sedation is generally safe, it carries potential risks, including respiratory depression, hypotension, and adverse reactions to sedative medications. Trained medical personnel monitor patients continuously to mitigate these risks.
Benefits of Unsedated Endoscopy
Some patients prefer to undergo endoscopy without sedation to avoid medication-related risks or because of personal preference [3].
Advantages of Unsedated Endoscopy
- Immediate Recovery: Patients can resume normal activities without waiting for sedation effects to wear off.
- No Sedation-Related Complications: Avoids risks such as respiratory depression, cardiovascular changes, or allergic reactions.
- Cost-Effective: Eliminates expenses related to anesthesia or sedation services.
- Patient Control: Some individuals prefer to remain fully aware during the procedure.
However, an unsedated endoscopy procedure can involve more discomfort, gag reflex, or anxiety, which may impact procedural tolerance and success.
Safety Considerations
Endoscopy exam is generally safe, whether performed with or without sedation [4]. Selecting the best approach requires consideration of patient health, anxiety level, and procedure complexity.
Risks of Endoscopy
| Feature | Sedated Endoscopy | Unsedated Endoscopy |
| Discomfort / Pain | Minimal | Moderate to high |
| Anxiety / Stress | Low | Moderate to high |
| Sedation-related risks | Respiratory depression, hypotension | None |
| Recovery time | 1–2 hours | Immediate |
| Procedural success | High | Slightly lower if patient cannot tolerate discomfort |
| Cost | Higher due to anesthesia | Lower |
Both procedures have high safety profiles in controlled clinical environments, but patient experience, comfort, and recovery differ.
Factors Influencing the Choice
1. Medical History
Patients with respiratory, cardiovascular, or neurological conditions may face higher risks during sedation. In these cases, unsedated endoscopy tests may be safer. Conversely, patients with high anxiety or previous difficulty tolerating endoscopy may benefit from sedation.
2. Pain Tolerance
Sedation is preferred for patients with low pain tolerance or heightened sensitivity to procedural discomfort. Unsedated endoscopy requires patients to manage mild gagging or discomfort.
3. Age and Comorbidities
Older adults or individuals with multiple health conditions may require careful monitoring if sedation is used. Healthy adults may safely undergo unsedated endoscopy in certain cases.
4. Procedure Complexity
Longer or more technical endoscopies, such as polyp removal or biopsy, are often easier to perform under sedation to improve success and minimize discomfort.
Preparing for Endoscopy
Preparation is critical for a safe and effective endoscopy procedure:
- Fasting: Required for upper endoscopy to reduce aspiration risk.
- Bowel Preparation: Required for colonoscopy to ensure clear visualization.
- Medication Review: Patients should inform providers of blood thinners, anticoagulants, or other medications.
- Hydration and Support: Proper hydration and having a support person improve safety and comfort.
Proper preparation reduces complications, shortens procedure time, and improves diagnostic accuracy [5].
Post-Procedure Considerations
After Sedated Endoscopy
- Recovery time of 1–2 hours is necessary.
- A responsible adult should accompany the patient home.
- Mild bloating or throat discomfort may occur but resolves quickly.
After Unsedated Endoscopy
- Patients can resume daily activities immediately.
- Mild discomfort or bloating may persist briefly.
- No restrictions on driving or returning to work.
Choosing Sedation vs. No Sedation
When Sedation May Be Recommended
- Anxiety, claustrophobia, or fear of procedures.
- Long or technically challenging endoscopy procedures.
- Low pain tolerance or previous incomplete endoscopy.
When Unsedated Endoscopy May Be Suitable
- Healthy patients seeking faster recovery.
- Desire to avoid sedation-related risks.
- Adequate tolerance for mild procedural discomfort.
Effectiveness of Endoscopy
Endoscopy is highly effective in diagnosing and preventing gastrointestinal diseases. Sedation may improve procedural comfort and success, while unsedated procedures reduce recovery time and avoid medication-related risks [6].
Both approaches require proper preparation, cooperation, and adherence to medical instructions to maximize safety and diagnostic accuracy.
Conclusion
Endoscopy is a safe and essential procedure, whether performed with sedation or without. Sedation improves comfort, reduces anxiety, and facilitates complex procedures, while unsedated endoscopy allows faster recovery and avoids medication-related risks.
Choosing the best approach depends on individual medical history, anxiety levels, pain tolerance, and procedure complexity. Discussing these factors with a healthcare provider ensures a safe, effective, and comfortable endoscopy experience.
Ultimately, understanding the benefits and risks of sedated versus unsedated endoscopy empowers patients to make informed decisions, ensuring optimal outcomes for digestive health and early disease detection.
References
- Peixoto, A. (2015). Biopsies in gastrointestinal endoscopy: When and how. PMC. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5580003/
- Issa, I. A., Lakis, R., & Issa, T. (2025). Sedation in endoscopy: Finding the balance between safety and efficacy. World Journal of Gastrointestinal Endoscopy, 17(8), 109695. https://doi.org/10.4253/wjge.v17.i8.109695
- Hassan, C., Rex, D. K., & Viale, E. (2013). Unsedated endoscopy: Feasibility, safety, and patient acceptance. Digestive and Liver Disease, 45(12), 989–993. https://doi.org/10.1016/j.dld.2013.06.003
- Dossa, F., Megetto, O., Yakubu, M., Zhang, D. D. Q., & Baxter, N. N. (2021). Sedation practices for routine gastrointestinal endoscopy: A systematic review of recommendations. BMC Gastroenterology, 21, 22. https://doi.org/10.1186/s12876-020-01561-z
- Lee, T. J. W., & Kaltenbach, T. (2018). Bowel preparation for colonoscopy: Current evidence and recommendations. Clinical Endoscopy, 51(6), 549–555. https://doi.org/10.5946/ce.2018.137
- Ai, Z.-L., Lan, C.-H., Fan, L.-L., Lan, L., Cao, Y., Li, P., Song, O., & Chen, D.-F. (2012). Unsedated transnasal upper gastrointestinal endoscopy has favorable diagnostic effectiveness, cardiopulmonary safety, and patient satisfaction compared with conventional or sedated endoscopy. Surgical Endoscopy, 26(12), 3565–3572. https://doi.org/10.1007/s00464-012-2367-4